Malaria’s Ticking Time Bomb
Source: Nature
Scientists are racing to stamp out the disease in southeast Asia before unstoppable strains spread.
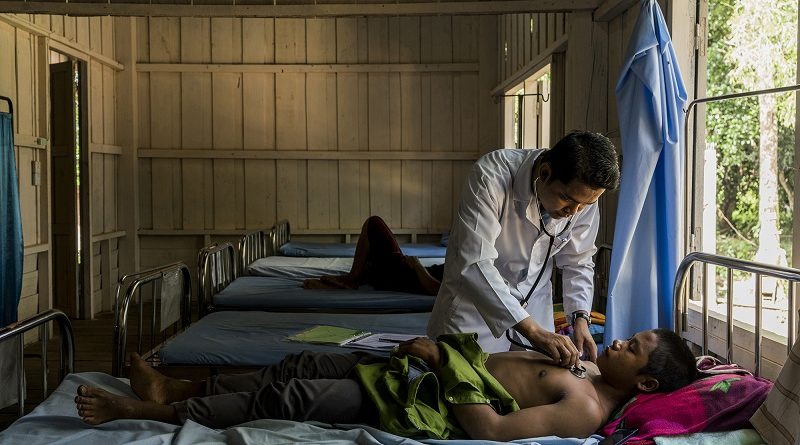
Throngs of men and women ventured into the forests of northeastern Cambodia in April, lured by a bumper crop of a rare tropical treat called samrong. After days of hiking through the wilderness, some of the travellers returned to their homes with a bounty of the wrinkled seeds, which fetch a high price as a special dessert or an ingredient in traditional Chinese medicine. But many soon fell ill. Khong Chhoem, a 56-year-old rice farmer, says the fevers hit him a few days after the expedition. His muscles hurt. His eyes hurt. He had unbearable nightmares. A health worker told Chhoem that he had tested positive for Plasmodium falciparum, the deadliest kind of malaria-causing parasite. But because a wave of malaria was sweeping through the region, medicine was in short supply. Chhoem eventually found a shop that carried the drugs he needed, and he recovered. But in the intervening days, mosquitoes probably sucked up the parasites in his blood and spread them to other people.
After years in decline, malaria infection rates seem to be on the rise in northeastern Cambodia, where people are moving deeper into lush, mosquito-ridden territories in search of timber and seasonal goods such as samrong (Scaphium affine). Their movements provide opportunities for P. falciparum — which requires both human and insect hosts — to thrive. There are other contributors as well, such as treatment delays that allow the parasites to linger and spread, and an alarming decline in the potency of gold-standard malaria drugs called artemisinin-based combination therapies (ACTs).

What happens next here matters for the entire world; malaria remains one of the biggest killers in low-income countries. Estimates of the number of deaths each year range from 450,000 to 720,000 — and ACT pills keep that toll from being much higher. And although southeast Asia accounts for just 7% of malaria cases worldwide, it has a notorious history as the breeding ground for strains of malaria parasites that resist every drug thrown at them and then spread to other regions.
In 2015, reports of drug resistance prompted the governments of five countries in the Greater Mekong Subregion — Cambodia, Thailand, Vietnam, Laos and Myanmar — to pledge to banish P. falciparum from the region by 2025. Together with the World Health Organization (WHO), the countries drew up plans and budgets. This year, the nations’ governments have committed US$41 million towards the effort; the Global Fund to Fight AIDS, Tuberculosis and Malaria also backed elimination efforts in the region, with a 3-year, $243-million grant. Donors such as the Bill & Melinda Gates Foundation and the Asian Development Bank will add more than $20 million to the fight this year.

But the rise of cases in northeastern Cambodia shows how difficult getting to zero will be — and how crucial. As long as P. falciparum exists, it can resurge. And the last parasites remaining are the hardest to find. They reside in the hinterlands, borderlands and war zones — and in people who show no signs of the disease. “Malaria is very clever — it hides out where you don’t know and comes back when you aren’t ready,” says Ladda Kajeechiwa, a malaria-programme manager at a branch of the Mahidol Oxford Tropical Medicine Research Unit (MORU) in Mae Sot, Thailand.
“Malaria is very clever — it hides out where you don’t know and comes back when you aren’t ready.”
To eliminate malaria, public-health officials are trying to cover the region with volunteers and health workers who can dispense malaria drugs promptly, and report any signs of an upsurge. They are also looking to researchers for tools that can forestall drug resistance, technologies that improve detection of the parasite, and evidence on strategies for rooting it out. The pressure is on. “Everybody has fears of malaria resurgence,” says Myaing Nyunt, a malaria researcher at Duke Global Health Institute in Durham, North Carolina. She worries that donors will tire of the cause, and that the people in the Greater Mekong region will grow to resent the obsession with malaria when they have more pressing needs. Yet if the effort lets up, malaria will roar back.
“That is why it is so important to eliminate it as quickly as possible,” Myaing Nyunt says.

The rise of resistance
The drug artemisinin is the gold-standard cure for malaria, but parasites that cause the disease have evolved mutations that can beat the medication.
rug resistance has a way of growing from a nuisance to a serious problem. Although an incompletely cleared infection might not kill a person, the parasites that survive can go on to infect others and their lineage grows stronger. To stay a step ahead of resistance, researchers at MORU renovated a dilapidated clinic in Siem Pang in northeastern Cambodia earlier this year. They are expanding a trial to test a combination of artemisinin with two partner drugs, rather than one. That combination should kill parasites that haven’t yet made it to the triple-resistant stage. But trial leader Arjen Dondorp, deputy director of MORU in Bangkok, says that the only certain way to halt resistance is to rid the Mekong region of malaria altogether. At the moment, the WHO considers elimination feasible because there are relatively few infections in southeast Asia. But the opportunity to do so won’t last long: as ACTs start failing, case numbers will rise. “This is the scenario we predicted and now we see it unfolding in Cambodia,” Dondorp says.
To hasten the elimination of P. falciparum in the region, public-health officials in the five countries have promised to strengthen the basic mechanisms of malaria control, which include maintaining a steady force of health workers. But gaps remain in this system, particularly in Cambodia and Myanmar, which are among the poorest countries in Asia. To help them, Benjamin Rolfe, head of the Asia Pacific Leaders Malaria Alliance in Singapore, has been garnering funds and political support throughout Asia. “We are so close to the end game that it is not good business sense to let drug resistance happen,” Rolfe says. “If we do, all the investments we’ve made so far here and in Africa will amount to an incredible waste of money.”

A technician in Siem Pang prepares blood cells for shipment to Bangkok, where biologists will study the malaria parasites living in the cells.
A scourge in hiding
Recent findings suggest that the task of elimination will be even harder than expected. Health workers typically diagnose malaria using a simple rapid diagnostic test (RDT): a pin-prick of blood is added to a test strip, which quickly turns red if it detects proteins from P. falciparum. The tests adequately distinguish malarial fevers from other infections. But Mallika Imwong, a molecular biologist at Mahidol University in Bangkok, wondered whether some people might carry too few parasites to make them ill — or to show up on a RDT. To find out, she fished for parasite DNA in vials of blood shipped from Cambodia, Myanmar and Vietnam, using a sensitive method called real-time polymerase chain reaction (PCR). In 2015, she reported7 that only one-quarter of Plasmodium infections were detected by the usual RDT on average. The disparity was at times remarkable. “I was really surprised,” says Imwong. “In one village, only 4% or 5% of the people were positive with RDTs, but 68% were infected.”
Researchers have not yet discovered how or why the parasites can persist at low levels in a person’s bloodstream. Whatever the reason, there are signs8 that these covert microbes multiply when conditions are right — such as when the rainy season starts.
Knowing that silent infections exist is one thing, but actually finding them is quite another. Health officials say it is unrealistic to conduct PCR analyses on vials of blood collected across the Greater Mekong Subregion. Rather, health workers need something like a rapid diagnostic test that requires no refrigeration, lab equipment or special training, but that can detect parasites even when they are not abundant.
In central Myanmar, a roving team of doctors, researchers and technicians are piloting one such technology. Thura Htay, a young physician and public-health researcher swerves on his motorcycle over rugged red-dirt roads with a green plastic supply bag gripped between his thighs. He is pensive, overseeing his group on its mission to collect pin-pricks of blood from 357 people in 3 remote villages by the end of the day. In these mountains, the things most likely to thwart the mission are flash floods and signs of wild elephants. (When startled by the sound of motorbikes, the animals sometimes attack people, homes and farms.)

Today, the path remains clear and the team arrives at the Shwe Kyin village before noon. A few dozen people linger on a concrete platform, where tables, chairs and bowls of pickled tea leaves, fried nuts and sweets have been neatly arranged in anticipation of the team’s visit. Although no one from the village has been diagnosed with malaria this year, Thura Htay says, “I want to know if asymptomatic malaria is here”.
A teacher in a rhinestone-studded top holds out her finger to a team member. He pricks it and places a drop of blood onto a conventional diagnostic test, and then onto an experimental version that the team is assessing to see whether it is more sensitive. Then he pricks another finger and presses it against two kinds of filter paper — one intended to capture DNA, and the other, proteins. The team swiftly hangs the papers on a clothes line to dry.
The teacher, Khin Zar Lwin, says she’s happy to help scientists learn about her village, but the emphasis on malaria by this and other groups feels like overkill; few people here get the disease, and there are other pressing health concerns. Pregnant women and elderly people who need urgent care, for example, must travel for hours on foot and then by boat down a tumultuous river to reach the nearest hospital, in the town of Singu.
In the late afternoon, the team packages the tests and blood spots into coolers strapped to the back of motorcycles, and returns to a concrete building in Singu. Team members hang the papers in a pair of cupboards, cooled and screened off to protect against mould and flies. Thura Htay sleeps on a bed beside them to ensure they are safe.
Every few weeks, the team ships samples to a renovated lab at the government’s Department of Medical Research in Yangon. There, researchers compare the results of the two rapid diagnostic tests with results from a PCR analysis on blood spots collected on one of the filter papers.
By the end of this year, Thura Htay — and his boss, Myaing Nyunt — will know whether the new diagnostic tests can be used to map out the regions where symptomatic and asymptomatic malaria occur. Such ‘hotspot’ maps will help officials to decide on elimination strategies for different regions. But the question remains of how to handle communities with hidden parasites. One possible answer comes from eastern Myanmar.
A few years ago, researchers mapped the malaria hotspots in Karen, a state along Myanmar’s border with Thailand that has resisted government rule since the country gained independence from Britain seven decades ago. (A symbol of that is its rejection of the state’s official name, Kayin.) Conflict has made many residents mistrustful of outsiders. But when MORU’s Ladda Kajeechiwa visited one of the hotspots in May this year, an old man in the village of Ta Oo Hta greeted her warmly.
The man, Bo Lay, recalls the toll that malaria took during the community’s darkest days. Burmese troops and armed groups attacked Ta Oo Hta several times, he says, and burnt it to ashes at least once. Each bout of violence drove people into the mountains, where they slept among the snakes and leeches. Those who became severely ill with malaria trekked through the jungle and crossed the Moei River to refugee clinics along the Thai border in Mae Sot. “Sometimes they died along the way,” he says.
Bo Lay was glad when he heard about MORU’s plan to wipe out malaria, and he discussed it with his neighbours, easing their suspicions of outsiders asking to draw blood and deliver drugs. This plan consisted of controlling malaria — and then pressing the accelerator on elimination. Beginning in 2014, MORU and other local organizations strengthened a network of 1,222 village malaria workers by training and paying them to treat and report any malaria cases that they find. In addition, they analysed blood samples across the state with PCR to find pockets of malaria. They then asked every healthy person in a hotspot — about 4% of Karen’s population — to swallow ACTs once a month for three months9. In surveys after the intervention, the researchers found that the incidence of malaria in the state had dropped by 90%. The only stronghold of the disease is in a rugged region in the north, where armed separatist groups rarely accept outside interventions.
“We have strong evidence that elimination can happen,” says François Nosten, a French researcher who founded MORU’s facility in Mae Sot, the Shoklo Malaria Research Unit, in 1986. But to his frustration, governments in the region have put mass-drug-administration strategies on hold for a number of reasons.

For instance, it takes a great deal of work to convince people who don’t feel ill to take medicines that can cause fatigue and nausea, and it requires funds to pay and organize health workers to survey populations for the parasite and distribute drugs. If a significant number of people don’t take the full course of therapy, parasite reservoirs remain — and some researchers fear that this situation could foster drug resistance.
Karen’s nearly disease-free status remains tenuous as long as malaria exists in the broader region. And its defence against imported cases relies on continued international aid because there is no stable health system in Karen. At the moment, the Wellcome Trust, the Global Fund and the Bill & Melinda Gates Foundation provide funds for malaria workers that ensure that any cases that pop up in the state are treated before the parasites have a chance to spread. But if donors put their funds elsewhere — or fighting breaks out again in Karen, as it has in the past — the system will fall apart and malaria will resurge. “The NGOs [non-governmental organizations] could pull out, the political situation is unstable,” Kajeechiwa says. “We work day by day, year by year, without guarantees on what happens tomorrow.”
A similar fragility exists in other states along Myanmar’s border, such as Kachin in the north and Rakhine in the west, the site of the ongoing Rohingya crisis. Since August 2017, more than half a million members of the Muslim Rohingya ethnic group have fled killings, arson and rape at the hands of Myanmar’s troops and nationalistic Buddhists. In these areas of the country, aid organizations and private clinics handle malaria because the public-health system is fractured. That concern resonates with Saw Nay Htoo, programme director of the Burma Medical Association, a non-profit organization working with minority ethnic groups. In an office in Mae Sot where vines penetrate the panelled ceiling, he says: “We want to eliminate malaria, but first we need peace.”

The last mile
Myaing Nyunt believes the common enemy of malaria could help to unite warring factions. She manifests that hope. A political dissident who fled from Myanmar’s military government in 1988, Myaing Nyunt now works with government researchers there. Squeezed into the back seat of a jeep beside Zaw Lin, an official in Myanmar’s Vector-Borne Disease Control department in Nay Pyi Taw, she explains why she decided to partner with researchers who are part of a government that has been accused of human-rights violations. Because there is no quick fix for malaria — no powerful vaccine — the fight against the disease requires a sustainable health system. As a scientist, she says she can develop top-notch malaria-elimination approaches and tools, but those won’t matter if governments do not put them into practice.
Always frank, Nyunt says that the decision to work closely with the government has made her research slow and hard. There are bureaucratic meetings to attend, labs to be built from scratch and students who are in need of long-term mentorship and stipends. “We are talking about a health system that has been underfunded and underdeveloped since the 1960s, and that’s not going to change overnight,” she says. “But you have to do it this way because changes must come from within.”
“We want to eliminate malaria, but first we need peace.”
If the new diagnostic that she and Thura Htay are road-testing in central Myanmar works, Zaw Lin will help the government to decide whether to pre-emptively distribute ACTs in hotspots, as was done in Karen, or to routinely screen people in those places with the new test, and treat those who test positive. He doesn’t shy away from talking about the country’s conflicts. In addition to political instability, he and other public-health officials find themselves pushing to sustain enthusiasm for their mission amid other health concerns. But he has seen at first hand how malaria bounces back if it’s not obliterated. It resurged in Myanmar in the 1990s, just as it seems to be doing in Cambodia and several other countries now.
Losing inertia in the Mekong region, the motherland of drug resistance, could be a disaster. “This is the last-mile challenge in front of us,” Zaw Lin says. “If we don’t eliminate malaria, deaths can shoot up like a hidden bomb.”